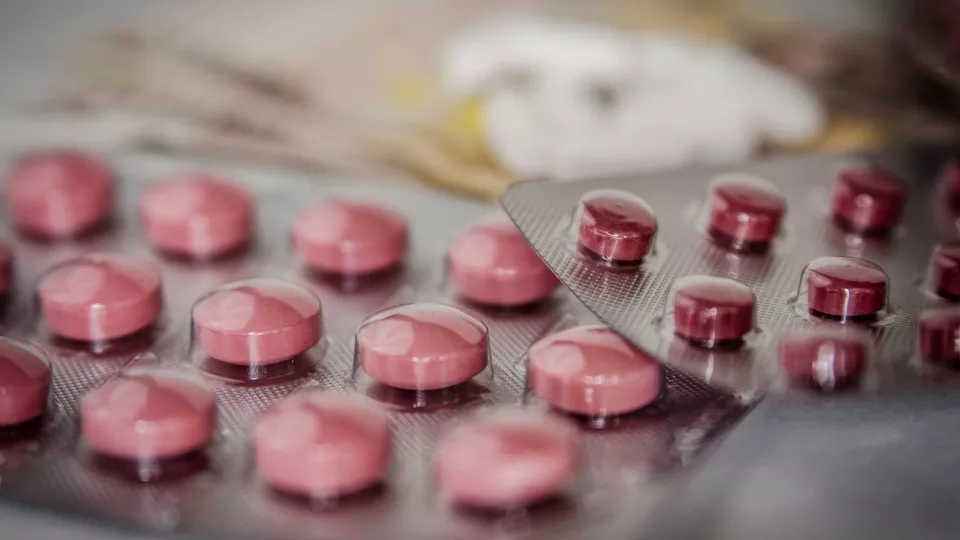
A recent study from England and Sweden (Lund University) has investigated the number of patients with knee osteoarthritis having required treatment with opioids in the years prior to total knee replacement. Opioids are a group of strong painkillers including Morphine, Oxycodone, Tramadol and Citodon. Opioids should be used sparingly since there is a risk of addiction at higher doses and/or long-term use. Furthermore, opioids have many side effects, some of which may be fatal.
In the present study, opioid use in over 50,000 patients with knee osteoarthritis was examined 10 years prior to the patients undergoing total knee replacement. The study showed opioid use steadily increasing between 10 and 2 years prior to surgery, and then sharply rose in the remaining 2 years before surgery. The use of opioids is not the first-line treatment for osteoarthritis and should be reserved for severe pain treatment where other treatments, including non-addictive drugs, have not given sufficient effect, or when a patient is unable to use other medication. Since osteoarthritis often deteriorates over time, it is not surprising that more patients were treated with opioids as the condition progressed. The authors of the study believe that the reason for opioid use increasing more rapidly in the two years preceding surgery was that some patients’ pain then was so severe that there were no viable alternatives to initiating treatment with opioids; this might have been an indication that the patient needed a referral for knee replacement surgery.
When comparing opioid use between the patients in Sweden and England, it became clear that the total proportion of patients treated with opioids was higher in England than in Sweden. However, the patients in Sweden were more often treated with stronger (more potent) opioids, whilst the patients in England more often were treated with weak opioids. The authors believe the difference in opioid strength between the countries partly stems from the fact that England offers more weak opioids to choose from, and that the tradition of which drugs are most often prescribed differs between the countries.
The study states that the number of patients with knee osteoarthritis who are treated with opioids is substantial, considering that opioids should only be used in exceptional cases. The authors believe that there is a need for better treatment alternatives for osteoarthritis, noting that some of the patients may have been deemed appropriate for surgery earlier in the process instead of being treated with strong painkillers.
Read the whole study here.